Assist. Prof.
Dr. Muhammad Shoaib Zafar
- Psychiatrist, Addiction Specialist
- M.B.B.S, M.D. (Psychiatry), B.Sc, Addiction Specialist
- 17 Years of Experience
Home » Psychiatrist
Psychological Factors in Obesity & Weight Management
- Written By Shoaib Zafar
- Date: 16-04-2026

When discussing obesity, most people think about calories, exercise, or metabolism. However, long-term weight gain is often deeply connected to emotional health, stress patterns, and behavioral habits.
In many patients across Lahore, weight challenges are not simply about diet — they are closely linked with mood, coping mechanisms, sleep, and stress levels.
Understanding the psychological dimension is essential for sustainable results.
Meaning In Urdu:
موٹاپے میں نفسیاتی عوامل جیسے اسٹریس، ڈپریشن اور ایموشنل ایٹنگ اہم کردار ادا کرتے ہیں، جس کی وجہ سے انسان ضرورت سے زیادہ کھانا کھاتا ہے۔
وزن کم کرنے کے لیے صرف ڈائٹ نہیں بلکہ ذہنی صحت، مثبت سوچ اور اسٹریس کنٹرول بھی بے حد ضروری ہے۔
Table of Contents:
- What are the Causes of Tired Eyes?
- Digital Eye Strain
- Insufficient Sleep
- What Happens to the Eyes with Untreated Tiredness?
- Eye Strain
- Increased Risk of Eye Infections
- Treatment and Management
- Conclusion
Emotional Eating: When Food Becomes a Coping Tool
Many individuals eat not because of hunger, but because of emotional triggers such as:
- Stress from work or family responsibilities
- Loneliness or boredom
- Anger or frustration
- Fatigue
- Anxiety
Food, especially high-sugar and high-fat options, activates reward pathways in the brain. This temporarily reduces emotional discomfort. Over time, the brain learns to associate stress relief with eating.
This creates a repeating cycle:
Stress → Eating →Temporary Relief → Guilt → Stress → Repeat
Without addressing this emotional loop, dieting efforts often fail.
Depression and Its Impact on Weight
Depression can influence weight in multiple ways:
- Reduced motivation to exercise
- Increased craving for carbohydrates
- Sleep disturbances
- Emotional overeating
- Low energy levels
Some individuals gain weight due to inactivity, while others use food for comfort. In addition, certain psychiatric medications may contribute to weight gain if not carefully selected and monitored.
Treating underlying depression often improves eating patterns and lifestyle consistency.
Anxiety, Stress, and Hormonal Changes
Chronic stress increases cortisol, a hormone that:
- Encourages abdominal fat storage
- Increases appetite
- Promotes sugar cravings
- Disrupts sleep
- Worsens insulin resistance
In busy urban environments like Lahore, long work hours, traffic stress, and financial pressure significantly contribute to stress-related weight gain.
Managing stress is therefore a medical necessity, not just a lifestyle suggestion.
Binge Eating Patterns
Some individuals experience episodes of uncontrolled eating. They may:
- Eat rapidly
- Consume large amounts in a short time
- Feel unable to stop
- Experience shame afterward
This pattern may indicate Binge Eating Disorder, a recognized psychiatric condition. Standard dieting alone does not treat this issue. Professional intervention is often required.
The Role of Trauma and Early Conditioning
Eating habits often develop in childhood. For some individuals:
- Food was used as a reward
- Emotional comfort came from eating
- Stress at home led to self-soothing through snacks
Unresolved emotional experiences can influence adult behavior unconsciously. Identifying these patterns helps break long-standing cycles.
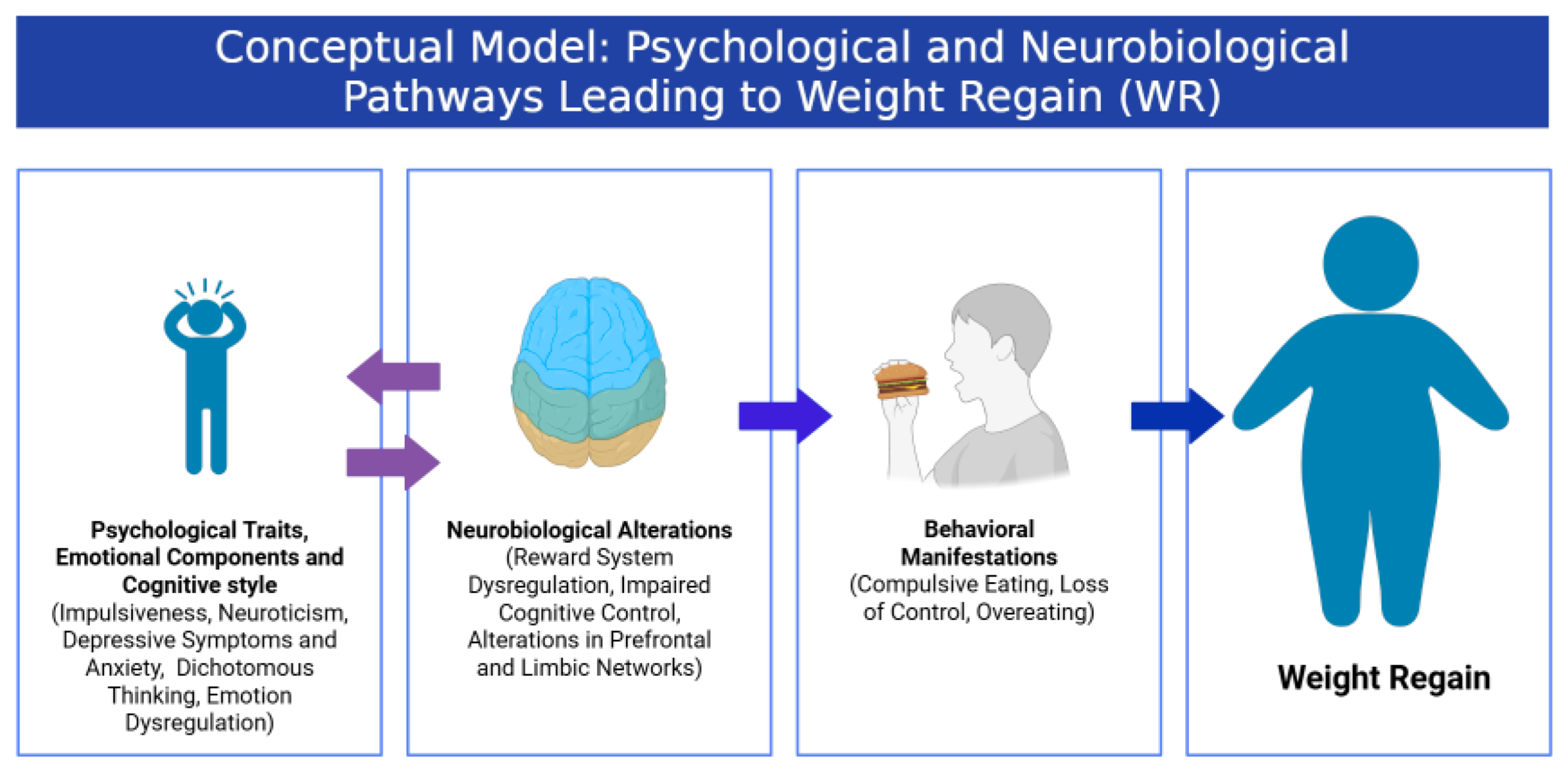
The Role of a Psychiatrist in Weight Management
A psychiatrist plays an important role when obesity is influenced by emotional or behavioral factors. Weight management becomes more effective when mental health is addressed alongside medical and nutritional care.
- Mental Health Assessment
- Medication Optimization
- Behavioral Therapy Strategies
- Addressing Food Addiction Patterns
- Motivation and Long-Term Maintenance
1. Mental Health Assessment
A psychiatrist evaluates:
- Mood disorders
- Anxiety disorders
- Sleep disturbances
- Emotional eating patterns
- Impulse control issues
- Medication-related weight effects
This helps identify hidden drivers of weight gain.
2. Medication Optimization
In selected cases, medication may be used to:
- Reduce binge frequency
- Improve impulse control
- Stabilize mood
- Improve sleep
- Support appetite regulation
Equally important, a psychiatrist ensures that prescribed psychiatric medications are chosen carefully to minimize unwanted weight gain.
Medication decisions are individualized and based on thorough evaluation.
3. Behavioral Therapy Strategies
Psychiatric guidance may include structured techniques such as:
- Cognitive Behavioral Therapy (CBT)
- Craving management tools
- Emotional regulation training
- Habit restructuring
- Mindful eating practices
These approaches help patients build sustainable habits rather than relying on short-term dieting.
4. Addressing Food Addiction Patterns
For some individuals, overeating resembles addictive behavior. Highly processed foods can stimulate dopamine pathways similar to other addictive substances.
A psychiatrist trained in addiction medicine can:
- Identify compulsive eating patterns
- Apply relapse-prevention strategies
- Develop structured coping mechanisms
- Prevent substitution behaviors
This is especially important when obesity coexists with substance use or addictive tendencies.
5. Motivation & Long-Term Maintenance
Sustained weight management requires psychological resilience.
A psychiatrist helps patients:
- Set realistic goals
- Manage setbacks without quitting
- Build self-discipline gradually
- Improve self-esteem
- Prevent relapse after weight loss
Weight management is not a short program — it is a behavioral transformation process.
Why Integrated Care Works Better
Programs that combine:
- Medical evaluation
- Nutritional planning
- Physical activity guidance
- Psychiatric support
Have significantly higher long-term success rates compared to diet-only approaches.
When emotional triggers are treated, the risk of weight regain decreases.
Final Perspective
Obesity should not be viewed as a lack of willpower. It is influenced by biological, environmental, and psychological factors.
Addressing emotional health alongside metabolic health leads to better, safer, and more sustainable outcomes.
If weight gain is associated with stress, mood changes, emotional eating, or repeated failed dieting attempts, a comprehensive evaluation that includes psychiatric assessment can provide clarity and direction.
Sustainable transformation begins with understanding the whole person — not just the number on the scale.